Overworked GPs in desperate need of help

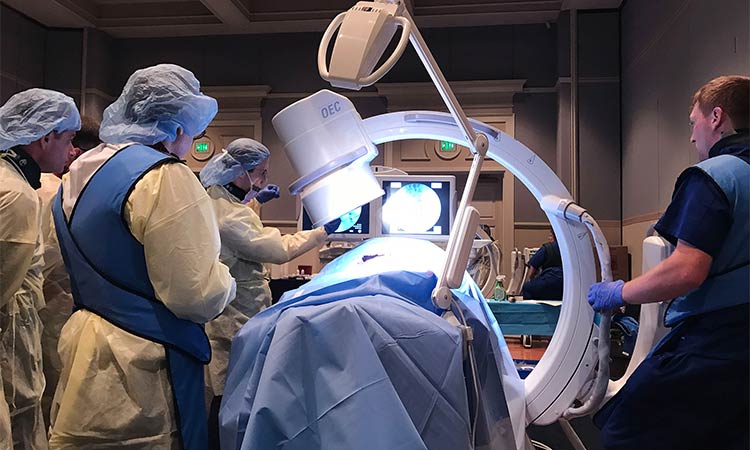
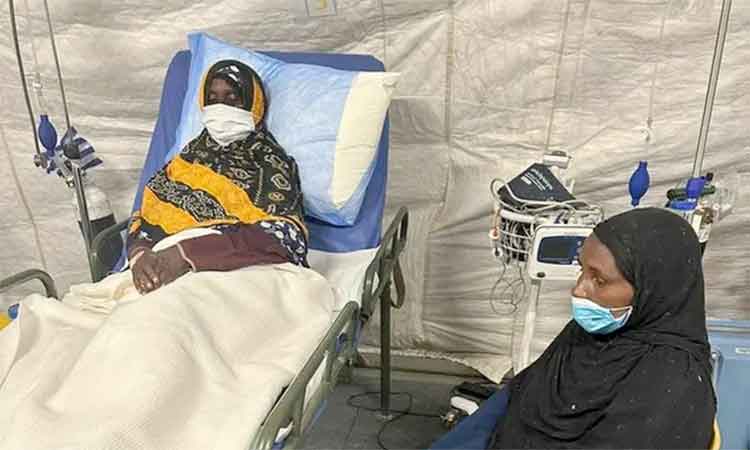
The photo has been used for illustrative purposes.
I work as a GP in a large practice in Bristol and my workload has reached unmanageable levels. I joined as a partner in 2010 when we served a population of 10,000 patients in a six doctor practice. But since then, while some surgeries have closed or merged in the city, no new practices have opened to take on the burden. We now have a 22,000 patient list and 15 doctors.
I always wanted to be a family doctor. The best thing has always been seeing the patients, following their journey and helping even in a small way. I work with a caring team and in a lovely building, even though we are packed like sardines to accommodate all our staff.
But I’ve been forced to work part-time — not through choice but necessity. The work has become physically and emotionally draining. The prevailing feeling is of being pulled in different directions with too much to do and not enough hours in the day.
A full day can be 12 hours long just to complete clinical work. After the last patient has left the building there is paperwork to read, referrals to type and prescriptions to sign. GPs have too many patient contacts a day (up to 41) including surgery or telephone appointments, and even Skype or email consultations.
Results and letters are often read at night when we are less likely to make high quality decisions. I usually undertake partnership and non-urgent tasks on my day off. Partners have the additional responsibilities of looking after the finances, managing the premises and sorting out staffing. We need to provide leadership, boost morale and give cover at times of staff shortages, despite often working at capacity ourselves and feeling like we are pouring from an empty cup.
Over recent years I have adjusted to this norm. At times I have felt exhausted and stressed. When I came back to work after maternity leave, I struggled to get home to feed the baby in the evening. My children are older now but I see little of them on the days when I’m at work and my husband looks after them. Likewise for him when he works long days in his hospital job. Sometimes it feels like we are two ships passing in the night.
Occasionally I come home and sit in my car outside the house to muster the energy to go in. There is no surplus emotion to make conversation with my family. All I want on those days is some food and sleep.
The exhaustion has left me sometimes inured to the reality of my work. I no longer lie awake worrying how busy my next on call will be or if I might make a mistake. At times I run late and am resigned to it – and just try not to think about the waiting room full of patients. Most patients understand. Some even say sorry that they have come to the doctors when the NHS is so stretched. They should not have to apologise.
Bottlenecks elsewhere in the system have made a big impact on our work. Cuts to pharmacy, sexual health, smoking and drug services have increased work load dramatically. Patients are increasingly dealing with the physical and psychological effects of deprivation and unfair social cuts.
The talking therapies required to deal with these problems have increasingly long waiting times, with many mental health issues now being dealt within in the community and increasingly falling on GP’s shoulders. There are more requests for sick notes, letters for school, colleges, benefits and housing agencies than I’ve ever seen. We are being asked to provide medical solutions to social problems.
A big issue has been difficulty in GP recruitment and this has affected us too, despite Bristol historically being a place where there is a surplus of doctors. We have tried innovative methods and now employ pharmacists, specialist nurses and paramedics. But as we drop one strand of work another seems to take its place, with little slack in the system.
Despite the hit it’s taken, I truly believe that general practice remains the bedrock of NHS. We must preserve what is good about it – at its best it provides safe, personalised evidence-based and holistic care.
But before we can look after patients we must self-care with our own “pulse check”. Highlighting our spiralling workload is the first step. We can no longer turn a blind eye – now is the time for GPs and the health service to work together to actively manage safe working limits.